
D-Day
Dear Members of the Baylor College of Medicine Community,
This week’s message may be slightly longer than usual, but I hope you will read it to the end. As the viral dynamics continue to improve in and around Houston, I want to pause to recognize a group that has borne a disproportionate brunt of pandemic-induced pain – our front-line health care providers (HCPs). Theirs is a compelling story.
Before I proceed, I will very briefly mention this week’s data. Our “R(t)” value is less than one (so we are winning). Hospital COVID-19 related census levels continue to drop steadily. The rate of new community cases is declining, albeit more slowly than anyone would like. The percentage of people with positive tests is declining. This is all favorable news. If you are not familiar with some of these terms or concepts, please refer to last week’s message for more details.
Things are looking up, but I must revisit a persistent theme in these messages: We must remain vigilant; we cannot become complacent. Mask, distance, and avoid crowds. Settle in for the long haul because we will need to live cautiously for months if we are going to be able to open up schools and maintain something that approximates our pre-COVID life. Again, refer to last week’s message for more details.
Now, on to front-line HCPs.
Every one of us has suffered, to varying degrees, during this pandemic. I have two new granddaughters, one born in September, and the other in June. I consider them both pandemic babies, born in a strange time. My younger granddaughter is named after her great-great aunt, who was an Army nurse, and part of the mobile medical response team that landed with the D-Day invasion in World War II. She has since passed away, but in all the years I knew her, I never heard her talk of her experience. I suspect it was horrific. Everyone in the United States suffered during WWII. There was fear of a mainland invasion, rationing of food, coffee and fuel, and shortages of rubber directed to the war effort. However, given that during D-Day almost 3,000 Americans died, and four times that number were wounded, most would agree that the suffering of the many back home did not compare with the experience of those who stormed the beaches.
Have I suffered during the pandemic? The honest answer is “yes, but…”
Yes. I have worked a little harder than normal. In welcoming our pandemic babies to the family, we have cancelled baby showers and missed a large family gathering for a baptism. We have not been able to jump on a plane for a quick visit. Everything is a little more complicated, and a little less convenient. To be sure, we feel fortunate that we have not suffered loss of livelihood, or health, or life – as many have.
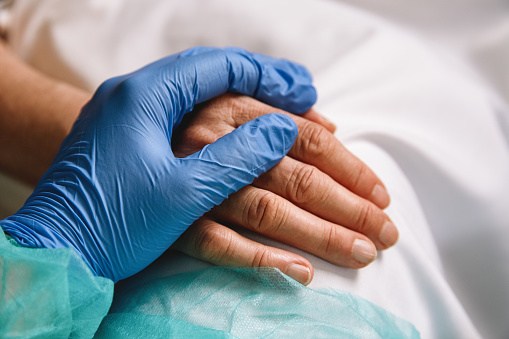
So we have suffered, but not to the extent of our front-line HCPs. In this SARS-COV-2 war, they are the soldiers, and our ICUs are the beaches of Normandy.
In preparation for this piece, I spoke to about a dozen inpatient front-line HCPs in several Baylor affiliates: Baylor St Luke’s Medical Center, Ben Taub Hospital, and Texas Children’s hospital. I spoke to intensivists and hospitalists; nurses and residents. I wish I could have spoken to them all, as they all had an important story to tell. What follows are a few of my questions to them. The responses are their words, not mine.
We have been dealing with this crisis now for six months. Tell me about your hardest day during that time, and what made it hard?
My hardest day was when I worked my first shift in a newly-designated “all-COVID” unit. All the patients were incredibly sick. There were multiple codes. I couldn’t leave one patient’s bedside long enough to attend to the next one. I went home and cried. I had to let it out. It was one of the worse days of my life.
Watching a young patient deteriorate before my eyes; seeing families devastated by the disease affecting multiple people.
We are a people called to care. In the early days, there was nothing we could do that seemed to help. It is hard when you can’t see a path forward.
I always try and take care of my people. I couldn’t help them.
I was worried about my family – that they would contract the disease.
It was physically grueling work. At any given time, 70% of our ICU patients were on a proning protocol.
It is very hard to take care of sick kids when both parents can’t visit, they can’t see my face though my mask, and I can’t sit on the edge of the bed.
What single word best describes your feeling on that day?
- Draining (multiple responses)
- Helplessness
- Overwhelmed
- Numb
- Anger (at the lack of resources in the early days, at the community at large for not taking this seriously)
- Despair
What did your team of health care providers do well?
We had a shared spirit, and collaborated broadly. It was one of the most rewarding experiences of my life.
I was proud of our new faculty. They were fearless.
Everyone was committed. Everyone sacrificed family responsibilities, vacation time. We all worked long hours.
We really rose to support each other. I was incredibly impressed and proud. Teamwork.
We adapted rapidly, and learned quickly. We became masters of data-driven micro-innovation. We are better for this experience.
Even though everyone was already incredibly busy, we held frequent Zoom meetings with regional hospitals to review cases and treatment protocols. We felt an obligation to help build capacity and improve quality across the region, just not in our hospital.
Imagine a time when COVID-19 is truly behind us. What is the single biggest lesson we should have learned from this experience?
Our health care community is incredibly valuable.
I cannot function without a great team around me. I have an overwhelming sense of humility, and gratitude for my colleagues.
We need to be ready next time.
Stockpile PPE.
Enhance our public health systems – earlier control, more effective contact tracing.
We have a leadership responsibility for the region.
Life is precious, but uncertain and fragile.
Putting others first is the best way to take care of yourself.
I hope we learn these lessons. I hope our front-line health care providers differ from the survivors of the Normandy invasion in one important way – I hope we continue to talk about these experiences. Experiences that have been incredibly hard, but at the same time affirming and formative. As one person commented, “talking about this has been very therapeutic.”
In closing, I want to express my admiration and gratitude to everyone in our professional community who has been on the front lines sacrificing to provide extraordinary care in extraordinary times to our families, friends and neighbors. May we never forget.
What would you like to communicate to a front-line health care provider? Using exactly five words, post to Twitter using the hashtag #COVIDThanksBCM, or send your five words to svpclinical@bcm.edu, and I will post some of your responses. Also, as many have asked, feel free to share this message broadly. You can copy and paste this link to email messages or social media: https://bit.ly/3277mrt.
So what are your five words of thanks? I will start, with apologies to Winston Churchill:
This was their finest hour.
James McDeavitt, M.D.
Senior Vice President and Dean of Clinical Affairs









There are currently no comments